What is Temporomandibular Joint Dysfunction?
Wed, Jan 16th, 2019
Temporomandibular Joint Dysfunction (a.k.a. TMJ Disorder or TMD) is a catch-all term that refers to any number of conditions that affect the temporomandibular joint.
What Are the Symptoms of Temporomandibular Joint Dysfunction?
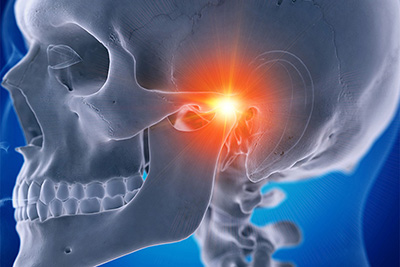
The temporomandibular joint connects the mandible (lower jawbone) to the skull; acting as a hinge, the temporomandibular joint allows for the movement required for chewing and talking. When the temporomandibular joint isn’t functioning properly, teeth clash and muscles strain while performing daily tasks such as talking and chewing. This can result in a number of symptoms, including:
- Pain around your jaw joint(s), face, neck and shoulders
- Difficulty or a strained sensation when opening your mouth
- Lock-jaw that occurs when the mouth is open or closed
- A grating or clicking sensation (or even a popping sound) when moving the jaw
- A clashing of teeth when chewing
- Facial swelling, particularly around the jaw area or near the temporomandibular joint
- Reoccurring headaches or migraines, particularly that always seem to appear first thing in the morning
- Extreme discomfort when yawning
What Are the Causes of Temporomandibular Joint Dysfunction?
Because the temporomandibular joint combines sliding motions and a hinge action, the bones that interact to create such movements are covered in cartilage and separated by a small disk that acts as a shock absorber. Usually, the dynamic combination of the shock-absorbing disk and cartilage allows for smooth, natural movement of the mouth.
However, painful disorders can occur when the shock-absorbing disk erodes or moves out of proper alignment, the cartilage covering the joint becomes damaged due to arthritis or the joint itself is damaged as the result of trauma. That being said, there are many instances where the exact cause of a TMJ disorder is not entirely clear, even to experienced professionals.
Unfortunately, since there is no widely accepted, standardized test to accurately diagnose temporomandibular joint dysfunction your medical professional will take note of any symptoms you may be presenting, examine specific problem areas, take a detailed medical history, and may even recommend specialized imaging including x-rays or an MRI to better understand the possible causes of your discomfort.
What Are the Treatment Options for Temporomandibular Joint Dysfunction?
Your medical professional may recommend a number of solutions to treat your temporomandibular joint dysfunction. However, because the exact cause of temporomandibular joint dysfunction is unidentifiable in many cases, most medical professionals will err on the side of conservatism when attempting to treat your TMD.
Over-the-counter anti-inflammatory medicines, like ibuprofen, may provide short-term relief from your symptoms. Various dental applications may be used in conjunction with OTC medications as well. Stabilization splints or a bite guard, that fits over both the upper and lower teeth, may also provide relief. In the event that a stabilization splint is recommended as a treatment option, it is important to keep in mind that it should only be utilized for a short period of time, as long-term usage may cause permanent changes in bite alignment.
In some extreme cases, your medical professional may recommend a more aggressive, irreversible approach to treating your temporomandibular joint dysfunction. Surgical intervention may be necessary if the temporomandibular joint has become disintegrated beyond repair and requires an artificial implant; though, it is generally accepted that any sort of surgical intervention should only be considered as a last resort treatment option.
What is the Outlook for Those Suffering from Temporomandibular Joint Dysfunction?
In most cases, temporomandibular joint dysfunctions are not serious and the pain or discomfort that it causes can be managed, if not eliminated entirely, from self-care and simple lifestyle changes such as:
- Not chewing gum
- Eating only soft foods
- Avoiding clenching or tensing the jaw
- Avoiding any extreme jaw movements (exceptionally wide yawning, loud singing, etc.)
- Incorporating relaxation and stress-relieving techniques into your daily routine, to reduce the frequency or severity of teeth grinding or jaw clenching
- Applying ice or heat to the specific pain points
Keep in mind, every case is different. If your temporomandibular joint dysfunction symptoms continue to persist, or if your ability to move your jaw becomes extremely restricted, it is best to make an appointment with Dr. Arnold for a comprehensive TMD evaluation, so he can help diagnose the root of your pain and offer solutions to assist in eliminating it.